The Silent Health Crisis: How the West Is Getting Sicker, More Expensive, and Less Honest About It
Over the past decade, Western societies have developed a dangerous habit: confusing economic activity with real progress. Nowhere is this more visible than in healthcare.
Every month, headlines celebrate “strong job growth in healthcare.” Politicians point to hospitals hiring, clinics expanding, and insurance enrollment rising as signs of resilience. Financial media frames healthcare as a “defensive growth sector.” Investors treat it as a stable pillar of modern economies.
But almost no one asks the obvious question:
Why is healthcare growing so fast in the first place?
The uncomfortable answer is simple. It is not growing because societies are becoming healthier. It is growing because people are getting sicker. Earlier. More frequently. More chronically. More expensively.
We are building more hospitals, hiring more nurses, training more therapists, expanding more insurance networks not because we are winning the health battle, but because we are losing it.
This is not a healthcare system problem alone. It is a civilization health problem.
1. The Job Growth Illusion: When “Growth” Means Decline
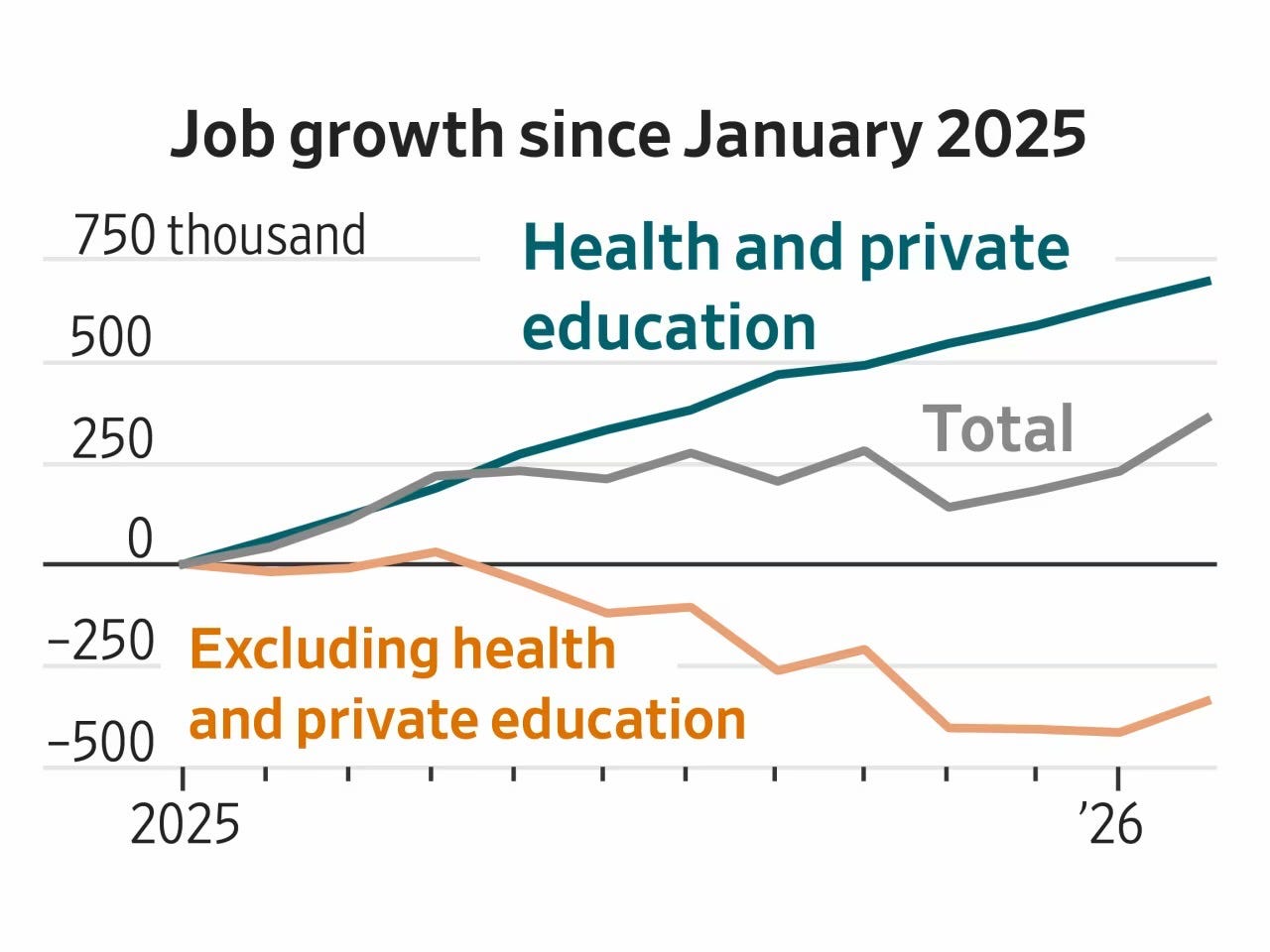
A 2026 analysis by the Washington Post (“Health-Care Industry Fuels Employment Growth,” February 2026) highlighted that more than 40 percent of net job creation in the US since early 2025 came from healthcare and private education.
At first glance, this looks positive.
In reality, it is alarming.
Between January 2025 and late 2026:
• Healthcare added roughly 650,000 jobs in the US
• Manufacturing added fewer than 100,000
• Technology employment stagnated
• Real wage growth slowed
Healthcare became the largest single engine of employment not because productivity surged, but because demand exploded.
Demand driven by illness.
According to the Bureau of Labor Statistics, healthcare employment has grown at nearly twice the rate of overall employment since 2015. Over the same period, life expectancy stagnated and then declined.
That is not coincidence. That is correlation.
A healthy society does not need exponential medical labor. A sick society does.
2. Life Expectancy: The Reversal Nobody Wants to Discuss
For most of the 20th century, life expectancy in Western countries rose steadily. It was one of the clearest indicators of progress.
Then something changed.
In the US:
• 2014: 78.9 years
• 2019: 78.8 years
• 2021: 76.1 years
• 2023: 76.4 years
According to CDC and National Center for Health Statistics reports.
After COVID, some decline was expected. What was not expected was the failure to rebound.
In peer countries:
• UK life expectancy plateaued after 2011
• Germany saw stagnation since mid-2010s
• France slowed dramatically
• Scandinavia decelerated
OECD Health Statistics, 2024 and 2025.
For the first time in modern history, technological advancement and medical spending are no longer translating into longer lives.
We are spending more. Employing more. Treating more.
And living less.
3. Chronic Disease: The New Normal
The real driver of healthcare expansion is not acute illness. It is chronic disease.
In the US:
• 60 percent of adults have at least one chronic condition
• 42 percent have two or more
• 12 percent have five or more
CDC Chronic Disease Report, 2024.
Major categories:
• Diabetes
• Cardiovascular disease
• Obesity-related disorders
• Autoimmune diseases
• Depression and anxiety
• Neurodegenerative conditions
Obesity alone affects over 42 percent of US adults. In 1990, it was under 15 percent.
Type 2 diabetes has tripled since 1980.
Hypertension affects nearly half of adults.
These are not “old-age” diseases anymore. They are appearing in people’s 30s and 40s.
We have normalized permanent illness.
4. Cancer Is Getting Younger
One of the most disturbing trends of the past decade is the rise of early-onset cancer.
According to studies published in The Lancet Oncology (2023–2025):
• Early-onset cancers (under 50) increased by ~80% globally since 1990
• Colorectal cancer in under-50s doubled in the US
• Breast cancer incidence in women under 40 rose sharply
• Thyroid and pancreatic cancers increased
American Cancer Society Report, 2025:
Colorectal cancer is now a leading cause of cancer death in men under 50.
This is unprecedented.
Cancer was once largely age-related. Now it is increasingly lifestyle-related, environment-related, metabolism-related.
Highly processed food. Microplastics. Endocrine disruptors. Sedentary life. Chronic inflammation.
We built an economy that produces disease efficiently.
5. The Mental Health Explosion
No part of healthcare illustrates societal decay more clearly than mental health.
In the US:
• 1 in 5 adults has a diagnosed mental illness
• Over 40% of high school students report persistent sadness
• Suicide is a leading cause of death under 35
CDC Youth Risk Survey, 2025.
Prescription data shows:
• Antidepressant use doubled since 2000
• ADHD medication usage tripled
• Anxiety prescriptions exploded post-2020
In Europe, similar patterns exist.
OECD Mental Health Review, 2024:
Depression and anxiety disorders cost Western economies over 4% of GDP annually.
This is not a temporary crisis. It is structural.
Loneliness. Digital addiction. Financial insecurity. Social fragmentation. Meaninglessness.
We medicate what is fundamentally cultural.
6. The Cost Catastrophe
Healthcare is not just growing. It is becoming financially unsustainable.
United States:
• 2000: $4,800 per capita
• 2010: $8,400
• 2020: $11,200
• 2024: $12,500+
CMS National Health Expenditure Report, 2025.
Total spending: Over $4.8 trillion annually.
Nearly 19% of GDP.
No other advanced economy comes close.
Germany: ~12%
UK: ~10%
France: ~11%
And outcomes are worse.
Medical debt is now the leading cause of personal bankruptcy in the US. Over 40% of adults carry healthcare-related debt.
Kaiser Family Foundation Survey, 2025.
Healthcare is becoming a financial disease on top of a physical one.
7. Media Silence: Why Nobody Connects the Dots
Mainstream media treats health issues in fragments.
Obesity article here. Mental health article there. Cancer story next week.
No synthesis.
No systemic framing.
No civilization-level analysis.
Why?
Because it challenges core narratives.
It challenges consumerism. Food systems. Pharma lobbying. Advertising. Tech addiction. Urban design. Work culture.
It questions whether “modern life” is actually healthy.
That is politically and economically inconvenient.
So instead, we celebrate “healthcare growth.”
We treat symptoms.
We avoid causes.
8. Blue Zones: The Exception That Proves the Rule
Journalists love writing about Blue Zones.
Sardinia. Okinawa. Ikaria. Nicoya.
People live long. Eat simply. Walk daily. Have strong communities.
And then we go back to McDonald’s.
These zones show what human biology is capable of under sane conditions.
They also show how abnormal Western life has become.
Ultra-processed food. 9-hour screen days. Chronic stress. Sleep deprivation. Social isolation.
We are running a mass experiment against our own biology.
And losing.
9. Healthcare Is Becoming Industrialized Illness Management
Modern healthcare is optimized for treatment volume, not health creation.
Hospitals optimize bed turnover.
Insurers optimize risk pools.
Pharma optimizes prescriptions.
Clinics optimize billing codes.
Nobody is paid primarily for keeping people healthy.
The system monetizes sickness.
Not deliberately. Structurally.
10. The Coming Wave: 2030 and Beyond
Demographics will make this worse.
By 2030:
• 1 in 5 Americans will be over 65
• Chronic disease prevalence will rise
• Alzheimer’s cases will double
• Cancer incidence will increase
• Diabetes cases will grow
Alzheimer’s Association Forecast, 2025.
This will overwhelm traditional systems.
Costs will rise faster than GDP.
Labor shortages will intensify.
Burnout will increase.
Something must change.
11. Why Most Insurers Are Not Ready
Most health insurers are legacy organizations.
High SG&A. Fragmented IT. Manual workflows. Paper-heavy operations. Slow claims processing. Poor data integration.
They grew in an era of low complexity.
That era is over.
Future healthcare requires:
• Real-time analytics
• AI-driven risk management
• Automated claims
• Preventive modeling
• Personalized care pathways
• Lean operations
Most incumbents cannot retrofit this easily.
Their systems are too old.
Their cultures too slow.
Their cost structures too heavy.
12. Oscar Health: Built for the Next Phase
This is where Oscar Health stands apart.
Unlike traditional insurers, Oscar was built as a technology-first health platform.
Key advantages:
1. Integrated Tech Stack
Oscar built its own operating system.
Claims. Member engagement. Provider coordination. Risk scoring. Data analytics.
Everything flows through one platform.
No patchwork.
No legacy silos.
2. Automation
High levels of automated claims processing.
Digital-first onboarding.
AI-powered triage.
Chat-based support.
Lower labor intensity.
3. Low SG&A Structure
Oscar consistently operates with lower administrative cost ratios than peers.
Automation replaces bureaucracy.
Software replaces headcount.
4. Data-Driven Risk Management
Oscar uses real-time data to:
• Predict cost drivers
• Identify high-risk members
• Intervene early
• Optimize networks
This is essential in a chronically ill society.
5. Preventive Orientation
Digital check-ins.
Care navigation.
Virtual primary care.
Proactive outreach.
Traditional insurers react. Oscar anticipates.
13. Why This Matters Strategically
The next decade will not reward insurers that simply process claims.
It will reward those that manage health complexity at scale.
Those that:
• Reduce friction
• Lower admin cost
• Improve outcomes
• Control risk
• Personalize care
Oscar is structurally aligned with this future.
It was designed for it.
14. The Bigger Picture: A Civilization Out of Balance
The healthcare crisis is not a technical problem.
It is a mirror.
It reflects:
• Poor nutrition systems
• Broken work-life balance
• Digital addiction
• Environmental toxicity
• Social fragmentation
• Meaning erosion
We are paying trillions to compensate for a dysfunctional way of living.
And calling it progress.
15. Conclusion: Health Is the Ultimate Infrastructure
Roads matter. Power grids matter. Data centers matter.
But nothing matters more than human health.
A society that cannot maintain the biological and psychological stability of its people is not sustainable.
Healthcare growth is not success.
It is warning.
The West is getting richer in machines and poorer in bodies.
Smarter in software and weaker in spirit.
More advanced and more fragile.
Until this is confronted honestly, costs will rise, lives will shorten, and systems will strain.
Companies like Oscar Health are preparing for the reality ahead.
Most institutions are still pretending it is not coming.
It is.
And it is already here.
The Tool I Use to Work Through This
When I analyze situations like this, I rely heavily on Fiscal.ai
It helps me:
• Normalize financials
• Cut through filings
• Model downside and upside scenarios
• Focus on structure instead of noise
I use it every day.


An American doctor summarised America’s healthcare system very succinctly for me: it does not exist to prevent illness, it exists to create and perpetuate illness so that a panoply of industries can get rich by treating the sick. The majority of the diseases afflicting Americans are self-inflicted (p.s. we Brits are almost just as bad). Don’t expect the food industry or politicians to rescue you - the answer lies in no small part in a healthier lifestyle, which is mostly a matter of assuming responsibility for one’s own health.
This piece is a sobering and important read that cuts through the comforting narrative that “healthcare growth” is automatically good news and reframes it as a symptom of a civilization-level health failure. I especially appreciate how it connects rising chronic illness, mental health struggles, and early-onset cancer to structural drivers: food systems, work culture, digital addiction, and environmental toxicity, rather than treating them as isolated data points.